The Vagus Nerve Is Having a Moment — But Does It Actually Work for Anxiety?
If you’ve spent any time on wellness social media accounts lately, you’ve almost certainly seen someone clipping a little device to their ear, humming in a low tone, or doing elaborate breathing exercises — all in the name of “stimulating the vagus nerve.” Vagus nerve stimulation is generating nearly a quarter of a million monthly searches, and wellness influencers are treating it like the secret key to unlocking calm, healing trauma, and rewiring the nervous system.
But is any of it real? Or is this just another wellness trend dressed up in neuroscience language to sell you a $200 ear clip?
The answer, as usual, is more interesting than either extreme. Here’s what the science actually says — and why it matters, especially if you or someone you love is navigating anxiety, trauma, or recovery.
First: What Actually Is the Vagus Nerve?
The vagus nerve is the longest cranial nerve in the body. It runs from your brainstem all the way down through your neck, chest, and abdomen, touching your heart, lungs, and gut along the way. Think of it as your body’s internal communication superhighway between your brain and your organs.
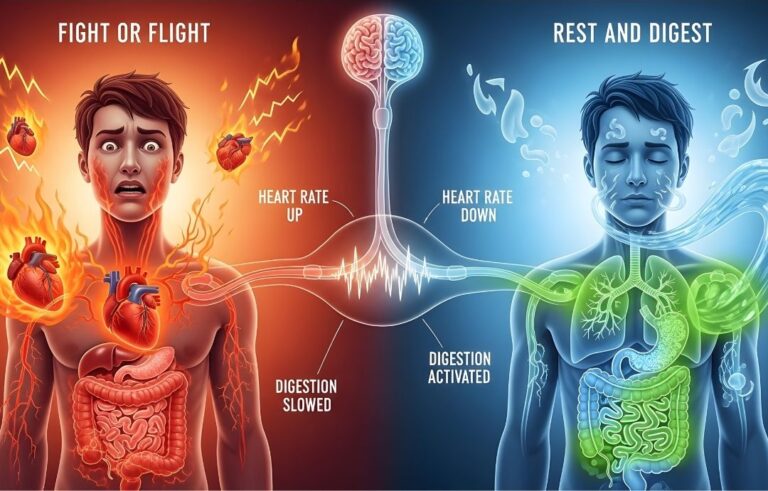
It’s also the nerve most responsible for activating your parasympathetic nervous system — the “rest and digest” mode that is the direct opposite of your “fight or flight” stress response. When the vagus nerve is functioning well, your body can shift out of alarm mode. When it’s not, you can get stuck in a loop of chronic anxiety, hypervigilance, and dysregulation.
For people dealing with anxiety, PTSD, addiction recovery, or trauma — all of which involve a nervous system that has been pushed past its limits — this is a very big deal.
So What Is “Vagus Nerve Stimulation”?
Vagus nerve stimulation (VNS) actually has two very different forms, and understanding the difference is key to cutting through the hype.
Clinical/Invasive VNS
This is a surgically implanted device — similar in concept to a pacemaker — that delivers electrical impulses directly to the vagus nerve. It has been FDA-approved for epilepsy and treatment-resistant depression for years, and the research behind it is substantial. A landmark 2025 clinical study from the University of Texas at Dallas and Baylor University Medical Center found that patients with treatment-resistant PTSD who received VNS therapy alongside prolonged exposure therapy experienced major, lasting improvements across anxiety, PTSD, and depression measures — and all nine participants in the trial were symptom-free for up to six months after therapy ended.
That’s the kind of result that normally doesn’t happen in PTSD research. “Rarely do they lose their PTSD diagnosis,” said Dr. Michael Kilgard of UT Dallas. “Typically, the majority will have this diagnosis for the rest of their lives.”
Non-Invasive / Transcutaneous VNS (tVNS)
This is the version you see all over social media. It involves stimulating the vagus nerve from the outside — most commonly through the ear (auricular stimulation), since a branch of the vagus nerve actually reaches the skin surface there. Devices range from ear clips that deliver mild electrical pulses to wearable neck devices. This is also where the DIY techniques come in: certain breathing patterns, cold water on the face, humming, and even gargling have all been proposed as ways to activate the vagus nerve non-invasively.
The research on non-invasive tVNS is still emerging, but it’s growing fast and the early results are genuinely encouraging.
What Does the Science Actually Say About Anxiety?
Here’s where it gets interesting. A 2025 randomized controlled trial found that a four-week course of vagus nerve stimulation significantly reduced anxiety, stress, and depression while also increasing confidence in participants. A separate 2025 single-blind trial involving 70 participants found that tVNS was effective in reducing both anxiety symptoms and perceived stress compared to sham stimulation. A 2025 meta-analysis of randomized controlled trials confirmed that transcutaneous VNS produces measurable improvements in sleep quality.
On the biological side, researchers understand fairly well why this might work. The vagus nerve connects to brain regions that are central to anxiety regulation — including the locus coeruleus, the amygdala, the hippocampus, and the orbitofrontal cortex. When it’s stimulated, it appears to modulate the release of norepinephrine and serotonin, two neurotransmitters closely tied to mood and anxiety. It also activates what’s called the cholinergic anti-inflammatory pathway, which helps suppress stress-related inflammation in the brain — a factor increasingly recognized as central to anxiety and depression.
For people in recovery from addiction, this matters enormously. Substance use disorders and anxiety are deeply intertwined — many people use substances precisely because their nervous system is stuck in overdrive. Anything that helps regulate that system from the root has real relevance to the recovery conversation.
But Let’s Be Honest About What We Don’t Know Yet
Good science requires honesty about limitations, and there are real ones here.
- Most tVNS studies are small. Many involve fewer than 100 participants, which means we need larger trials before drawing firm conclusions.
- Consumer devices vary wildly in quality, and not all of them actually deliver meaningful stimulation to the vagus nerve.
- The TikTok techniques — humming, gargling, cold water — are based on plausible biological logic, but have far less rigorous research behind them than electrical stimulation devices.
- Individual responses vary significantly, and VNS is not a replacement for therapy, medication, or other evidence-based treatment.
The bottom line: this is a real and promising area of research, not pseudoscience. But it’s also not a magic bullet, and the wellness world has a habit of getting ahead of the evidence.
The Free, Evidence-Adjacent Techniques Worth Trying
Even without a $200 device, there are several practices with plausible vagal benefits and good general evidence for calming the nervous system. None of these replace clinical treatment — but as daily tools for managing anxiety and supporting recovery, they’re worth knowing about.
Slow, Deep Breathing (Especially Long Exhales)
This is the most well-researched DIY technique. Breathing at a slow pace with an exhale that’s longer than your inhale (try 4 counts in, 6–8 counts out) activates the parasympathetic nervous system. It’s not magic — it’s physiology.
Cold Water Exposure
Splashing cold water on your face, or briefly submerging your face in cold water, triggers the diving reflex — a rapid drop in heart rate that activates the vagus nerve. It’s been used in dialectical behavior therapy (DBT) as a grounding technique for years.
Humming, Singing, or Gargling
These activate the muscles in the throat and larynx that are connected to vagal pathways. The evidence is preliminary, but the practices carry essentially zero risk and many people find them genuinely calming.
Mindfulness and Meditation
Long-term mindfulness practice has been shown to improve heart rate variability (HRV) — a key marker of vagal tone and nervous system flexibility. The vagus nerve connection is one of the reasons this works.
What This Means If You’re In Recovery or Supporting Someone Who Is
Anxiety is one of the most common drivers of substance use. It’s also one of the hardest things to manage in early recovery, when the brain’s reward and stress systems are actively recalibrating. The nervous system dysregulation that underlies both anxiety and addiction is real, measurable, and increasingly treatable.
Vagus nerve stimulation — both clinical and the gentler everyday practices — is one piece of a larger picture. It’s not a cure. But understanding that your nervous system can be worked with, not just endured, is itself a powerful shift in perspective.
If you’re curious about clinical VNS options, talk to your doctor or psychiatrist. If you’re looking for daily tools to support your nervous system, the breathing practices and cold water techniques above are free, safe, and worth building into your routine.
And if you’re watching vagus nerve content on TikTok and feeling cautiously hopeful — that instinct isn’t wrong. The science just asks you to pair it with realistic expectations.
Lindsey Glass is a self-help author and the founder of ReachOutRecovery.com. She is the author of the Mother Daughter Relationship Makeover series.
Check Out My Books!
Like us on Facebook
Follow us on Instagram
More Articles To Read